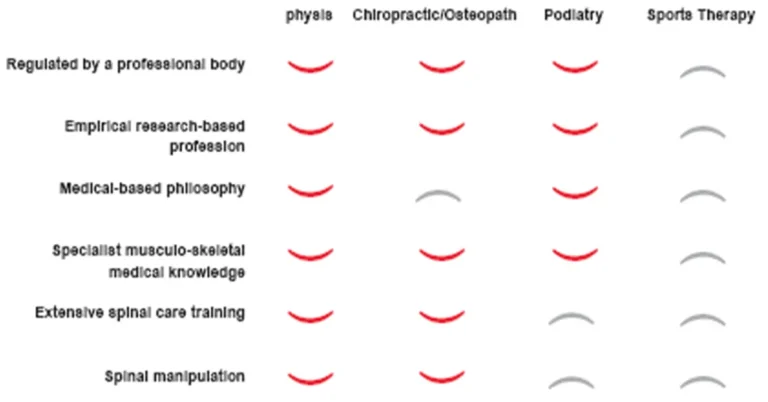
Physiotherapy, Chiropractic or Osteopathy. How do you choose?
Lets start with the difference between a physiotherapist, a chiropractor, and an osteopath?
This is a question we get asked all the time and one, which can produce widely different responses depending on your background. Below is our view, based, as ever, on the available evidence.
There are many similarities between the professions which include;
- we all treat musculoskeletal pain conditions;
- we all have protected titles, meaning that a therapist cannot call themselves an a Chiropractor, an Osteopath or a Physiotherapist, unless they have completed the relevant accredited course;
- we all have university based education.
Put simply, the main difference between a physiotherapist, a chiropractor and an osteopath is in the philosophy of each profession. However, there are also fundamental differences in the approach we take with people.
Chiropractors
Chiropractors will generally treat pain related problems using manipulation of the joints (adjustments), either of the spine or the limbs. Manipulation is a fast manual technique that takes the joints being treated to the end of their available range of motion. This is commonly viewed as a treatment with more risk to the individual that is not always necessary. Both Physiotherapists and Osteopaths will use manipulation, but it is generally, not seen as a first option in treatment as it is in Chiropractic. Also, the chiropractic philosophy relies on the belief that the cause of back pain lies with subluxations, or certain joints being ‘subluxed’ (not to be confused with the medical definition of a subluxation, which is the incomplete or partial dislocation of surfaces within a joint). This belief is controversial, even within the chiropractic profession, as a ‘chiropractic subluxation’ has never been shown to exist. If one had to define a Chiropractic subluxation, it could not be done within an objective scientific (evidence based) framework . In their defense Attorney David Chapman-Smith, Secretary-General of the World Federation of Chiropractic, has stated that “Medical critics have asked how there can be a subluxation if it cannot be seen on x-ray. The answer is that the chiropractic subluxation is essentially a functional entity, not structural, and is therefore no more visible on static x-ray than a limp or headache or any other functional problem’ (Wikipaedia, David Chapman-Smith (2000). “Principles and Goals of Chiropractic Care”. The Chiropractic Profession: Its Education, Practice, Research and Future Directions. NCMIC Group. pp. 160.ISBN 1-89273-402-8.) This stance may seem reasonable, but many chiropractors still endorse using static x-ray to identify the ‘chiropractic subluxations’. This obviously makes no sense when it is admitted that it is not visible on X-ray. Using X-ray in diagnosis of this sort has been condemned as dangerous, as it exposes individuals to levels of potentially carcinogenic radiation for no reason, as well as being of no use in the diagnosis of non-specific low back pain.
There are also issues regarding safety of chiropractic in the treatment of neck pain. Chiropractors are associated with more serious adverse reactions than other health professionals (E Ernst (2010). “Deaths after chiropractic: a review of published cases”. Int J Clinical Practice 64 (8): 1162–1165.). Whilst many Physiotherapists and Osteopaths will use manipulation of the cervical spine, Chiropractic treatments of the lower back may often involve neck manipulations. There is no evidence that manipulation of the cervical spine will have a positive effect on a person’s low back pain.
Although there is some evidence to suggest that chiropractic is as effective for low back pain as other mainstream treatments, Chiropractic has been labeled as quackery in relation to it’s claims regarding treatment of medical conditions such as asthma, ear ache, colic or sexual dysfunction (Trick or Treatment, Alternative medicine on trial S Singh, E Ernst 2008). This is simply because there is no evidence that it works for medical conditions, and there is no reasonable mechanism through which it should work, other than through placebo.
Osteopaths
Osteopathy is also a manual therapy based treatment of the musculoskeletal system, and like Chiropractic, there are divisions of Osteopathy that believe in the treatment of non-musculoskeletal medical conditions such as respiratory or digestive conditions through mobilization / manipulation of the spine. The inappropriate use of manual therapy for these types of conditions has been covered above.
Generally, Osteopaths will use manual, hands on techniques to restore structural alignment with the aim to improve pain and function. They commonly do this with more gentle techniques than manipulation, but can manipulate. The osteopathic philosophy is based upon the belief that in order for the body to be healthy, all body tissues are required to move according to their function. The Osteopathic philosophy maintains that it movement exists and is balanced then good health will follow. This absence of movement is assessed through manual palpation. For the most part this philosophy seems fairly rational and logical. However, when looking at pain related problems, in the spine for instance, structural symmetry rates very poorly in whether someone recovers well or not. Outcome is dependant more on a person’s belief about their spine, (Grotle M, Brox JI, Veierød MB, Glomsrød B, Lønn JH, Vøllestad NK. Clinical course and prognostic factors in acute low back pain: patients consulting primary care for the first time. Spine. 2005;30:976). A focus on the quantity of movement as being the underlying cause of pain related problems neglects the influence of the mind and its huge influence on whether someone even experiences pain or not. This clearly contradicts the current view in the management of all pain related conditions.
In certain areas of Osteopathy, such as Cranio-sacral Osteopathy, this structural approach has developed beyond rational anatomical science, since these areas either do not move (Adult cranium) or are certainly not detectable by physical palpation (Sacro-iliac joint, van der Wurff P, Hagmeijer RH, Meyne W. Clinical tests of the sacroiliac joint. A systemic methodological review. Part 1: reliability. Manual Therapy 2000a;5(1):30–6; van der Wurff P, Meyne W, Hagmeijer RH. Clinical tests of the sacroiliac joint. A systematic methodological review. Part 2: validity. Manual Therapy 2000b;5(2):89–96). Unfortunately, this area of Osteopathy has made its way into some physiotherapy circles. It is our belief that this type of treatment has no place within a science based profession.
Physiotherapists
Physiotherapy in the context of a private clinic for musculoskeletal pain conditions will often employ an approach that is described as bio-psycho-social meaning that treatment is directed to the person as a whole. This is claimed by many different therapies and professions, but in order to actually to do this, the therapist must have a philosophy and an approach to a problem that incorporates a broad skill set. With an ability to assess various different aspects of a problem, the cause can be more effectively identified, and then, efficiently dealt with. These areas requiring assessment for potential involvement include physical aspects such as joint mobility, muscle strength, muscle flexibility, nerve function and sensitivity, body posture, ergonomics, movement patterns, psychological aspects such as beliefs, attitudes, fears, anxiety, and stress, and social aspects such as work patterns, behaviours, and lifestyle. The management of chronic problems must incorporate more than just the physical aspects, and in order to prevent acute (recent) problems from becoming chronic (long term – over 3 months) these same bio-psycho-social aspects need to be addressed. There is good evidence that the psychological & social factors will determine how well someone recovers. These factors are more predictive of a good outcome than X-ray or MRI, so they should not be discounted. Physiotherapists at physis acknowledge the influence of all three aspects on pain, and are well equipped to deal, in the whole, with the majority of cases.
At physis our working philosophy is about keeping things simple and logical. It is hoped that by the end of your first session you will have a clear understanding of what the problem is (in real terms, not made up mumbo jumbo), and how you got yourself into this situation (ie, the underlying cause of the problem – which then allows you to prevent recurrences). Although in the majority of cases establishing a clear picture of a person’s problem is achievable in one session, sometimes it may take more than one. Knowledge IS power, and we aim to make you more knowledgeable about your condition, thus giving you more power to deal with it.
Frequently asked questions
Do you need an x-ray to treat your back or neck?
Generally speaking no. There may be a few select cases that might require clarification to rule out a specific serious pathology, but generally x-rays are completely unnecessary in aiding the treatment of simple neck and back pain. In fact because of the exposure to harmful radiation, it is recommended that you do not have an x-ray without a good clinical reason. This is also the stance of the General Chiropractic council, although their advice is vague and leaves considerable room for interpretation as far as what constitutes ‘clinical relevance’, hence the frequent use of X-rays by Chiropractors. Most X-rays will highlight the normal and natural changes which occur in joints due to the aging process, these changes to not indicate a reason for specific or long term therapy intervention. They specifically do not indicate the need for regular manipulative therapy to those joints.
Is neck manipulation safe?
This is an area of controversy between the manual therapy professions. Generally speaking the chiropractic profession’s stance is that it is perfectly safe as thousands of cervical manipulations occur every day. However, much of the research does show a risk of cervical artery damage with cervical manipulation (manipulation being defined as a fast, short movement of the body creating a ‘crack’ or cavitation, which is just gas forming in the joint) which has a risk of producing a stroke or even death. This risk of artery damage is estimated at 1 in 100,000 manipulations. In a review of the reported literature there have over 700 cases of serious complication documented, and it is accepted that the real occurrence of serious injury as a result of cervical manipulation is much higher (Ernst E, Canter PH, A systematic Review of Systematic reviews of spinal manipulation, J R Soc Med 2006, 99:192-6). There is weak to moderately strong evidence that supports causation (as opposed to statistical association) between cervical manipulative therapy and vertebrobasilar artery stroke (Miley ML, Wellik KE, Wingerchuk DM, Demaerschalk BM (2008). “Does cervical manipulative therapy cause vertebral artery dissection and stroke?”. Neurologist 14 (1): 66–73). Mobilisation does not share these risk factors and is a safe treatment. If the clinical presence shows a painful restriction of the cervical spine joints and that the therapist chooses manipulation as the preferred treatment approach, the risks of treatment must be fully discussed with patient and consent gained, before this treatment technique is used.
How does manipulating my neck help my low back pain?
There is no evidence that neck manipulation will have a positive impact on low back pain, and it does not make anatomical sense that the origins of low back pain would be within the cervical spine. So unless you can link a loss of range of motion in your neck directly to your low back pain, like ‘my pain comes on in my back when I turn my head’ there should be no justification for treating the back with cervical treatments, especially manipulations (see is neck manipulation safe?) which carry a specific patient risk. In short, don’t let your therapist crack your neck to ease your lower back pain, unless they make a very sensible case for it. Even then, mobilisation is safer.
I have been told my pelvis is out of alignment, can a manipulation put it back?
This is another area of controversy within the field of medicine where old belief systems are held simply because they have been around for a long time. There is no evidence to support the belief that the pelvic joints slip out of place. The pelvic joints are two of the most stable joints in the body. When the joints are stressed, the bone will fracture first before the joint is displaced! – they are extremely stable. Unfortunately however, this is a common story people are told, and yet the science behind this approach is very poor. There is some evidence to point to an increased movement of the front of the pelvis in relation to pregnancy related pelvic girdle pain, but there is a poor correlation between the movement and the pain, suggesting there are other underlying causes that are as yet poorly understood.
The pelvis remains a solid ring and any displacement is simply a tilting of the pelvis on the hip joints. This may be due to muscle tightness pulling up on one side. The therapy commonly offered works on the local soft tissues and how they effect the function of the stable pelvic ring rather than simply putting it back into place. Exercise therapy also often helps patients manage pain in this area. The belief that the pelvis twists or slips up on one side is very biomechanical in approach and does not fit within a biopsychosocial model. It can create fear, anxiety, hypervigilance and dependency, all of which have been shown to be predictors of a poor resolution. These aspects often make patients believe that it is the role of the therapist to put the pelvis back leading to prolonged patient contacts. Your body is strong & robust structure, and your pelvis is the most stable part of it! At physis we focus on improved function of the joints and muscles around the pelvis to allow any pelvic sensitivity to settle. This approach is more in keeping with the accepted human anatomy and pathology, as well as accurate movement studies (Sturesson et al (1989) Movements of the sacroiliac joints. A roentgen stereophotogrammetric analysis. Spine;14(2): 162–5. Sturesson B, (2000) A radiostereometric analysis of movements of the sacroiliac joints during the standing hip flexion test. Spine;25(3):364–8.
Do I need a long course of manipulation for my back problem?
There is no reasonable evidence available which supports the use of regular manipulations as being of general health benefit or prevention within the musculoskeletal system. There is evidence to suggest exercise, posture and function as being the best methods to manage long term issues.
Can manipulation really help my Asthma, or colic, or bed wetting?
There is no evidence that manual therapy of the spine helps in non-musculoskeletal problems like asthma, colic, bed wetting, painful menstrual cycle, high blood pressure, or depression for example. Any anecdotal benefits observed in this area are considered to be as a result of the placebo effect.
Should I send my child for cranial osteopathy?
The basis of this approach was developed by an osteopath in the 1930’s who believed a persons health was linked to small movements of the bones of the skull. Viewed from a scientific perspective, these observations have never been demonstrated and the principle of the approach is biologically implausible as the bones fuse in early childhood, and there is no causal link between the shape of the skull and a person’s health.
Will I not just get Transversus exercises at physio?
Definitely not! At physis we believe in good logical evidence based science. Unfortunately, physiotherapy and the fitness industry has been plagued by poor reasoning surrounding this abdominal muscle and its role in low back pain since the early 90’s and yet there is no convincing evidence that says exercise programmes to ‘re-activate’ this core muscle are any better for your lower back than any other form of exercise. The research in the early 90’s has been extrapolated far beyond its remit and whole industries have developed on the basis that this muscle is responsible for most lower back pain. This is obviously ridiculous, but many clinicians will follow this line of thought and push tranversus exercises, when there is actually very poor evidence to support this belief. Many fitness trainers also push the belief that your core is the root of many musculoskeletal problems; that if you have a good strong core you will not get back pain. This is not the case. In fact, there is some evidence to show that chronic low back pain patients tend to have more muscle activity than people without. This suggests that ‘engaging your core’ might not be that good for you! Everything in moderation!